One minute you're sitting on the couch, watching TV. The next, you can't catch your breath. No cough, no fever - just this overwhelming feeling that your lungs aren't working. If you've ever had this happen out of nowhere, especially if you've been sitting for hours or recently had surgery, you might be dealing with something far more serious than anxiety or asthma. This is the reality for thousands of people every year with pulmonary embolism - a blood clot blocking blood flow in the lungs.
It doesn't always come with warning signs. Many people think of heart attacks or pneumonia when they feel short of breath. But pulmonary embolism (PE) often hides in plain sight. In fact, 85% of confirmed cases start with sudden or worsening shortness of breath. That’s the number one red flag. And it’s not always dramatic. Sometimes it’s just climbing stairs that used to be easy. Or walking to the kitchen feels like running a marathon.
Where Do These Clots Come From?
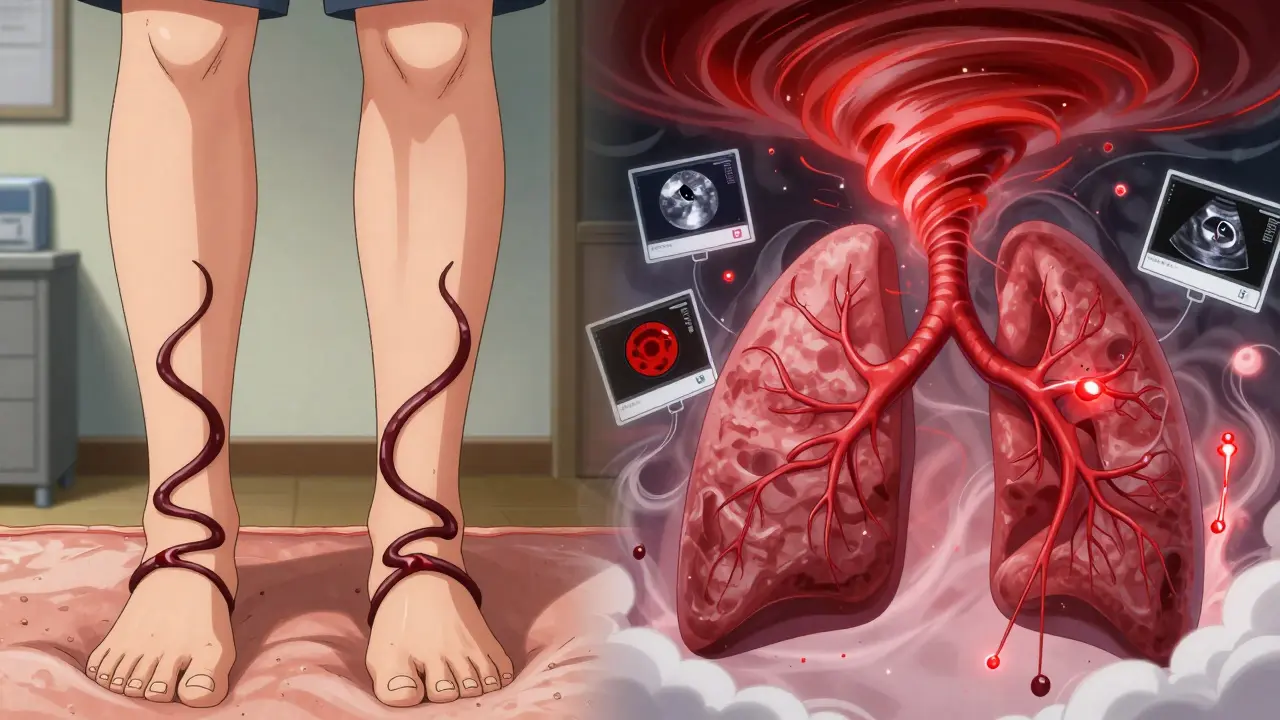
Most of the time, the clot doesn’t start in the lungs. It starts in the legs - usually deep in the veins, a condition called deep vein thrombosis (DVT). About 70% of pulmonary embolisms trace back to clots that broke loose from the lower limbs. Sitting for long flights, being bedridden after surgery, or even just being inactive for days can trigger this. The clot forms, loosens, and travels through the bloodstream until it gets stuck in the narrow arteries of the lungs.
Less common sources include clots from the arms, often after someone has had a central line or IV catheter placed. But leg clots are the main culprit. And once that clot reaches the lungs, it blocks oxygen from getting to the bloodstream. That’s why you feel like you’re suffocating - even if your chest looks perfectly normal.
What Else Should You Watch For?
Shortness of breath is the big one, but PE doesn’t show up with just one symptom. Here’s what else commonly happens:
- Chest pain - sharp, stabbing, and worse when you breathe in or cough. It’s often mistaken for a heart attack, but it’s tied to the lung tissue being irritated by the clot.
- Cough - happens in over half of cases. Sometimes it’s dry. In 23% of cases, you might cough up blood.
- Leg swelling - especially in one leg. This is the clue that a DVT might be the source.
- Fast heartbeat - over 100 beats per minute, even at rest.
- Fast breathing - more than 20 breaths per minute.
- Fainting - happens in about 1 in 7 cases. This usually means the clot is large and blocking major blood flow.
Some people get all of these. Others only get one or two. That’s why PE is so tricky. It doesn’t look like textbook pneumonia or asthma. It looks like something’s off - but doctors don’t always suspect it right away.
Why Diagnosis Gets Delayed
On average, patients visit healthcare providers 2.3 times before being correctly diagnosed with PE. That’s not rare. In a 2022 survey of 1,200 patients, 41% were first told they had pneumonia or asthma. One patient on a health forum described being told she had anxiety after three ER visits - until she passed out and a scan revealed a massive clot.
Why does this happen? Because the symptoms are too common. Shortness of breath happens with allergies, stress, COPD, even being out of shape. Doctors have to rule out the usual suspects first. And if a patient is young, healthy, or doesn’t have obvious risk factors, PE isn’t always the first thought.
But here’s the thing: if you have unexplained shortness of breath and no clear cause - especially if you’ve been inactive, had recent surgery, or have a history of blood clots - PE needs to be checked. Right away.
How Do Doctors Confirm It?
There’s no single test that catches every case. Diagnosis follows a step-by-step process based on risk, symptoms, and available tools.
Step 1: Clinical Scoring
Doctors use tools like the Wells Criteria or Geneva Score. These aren’t magic - they’re simple checklists. Things like: Is your heart rate over 100? Do you have leg swelling? Have you had cancer or surgery in the last 3 months? Each answer adds points. If the score is low, PE is unlikely. If it’s high, they move fast.
Step 2: D-dimer Test
This blood test looks for a substance released when clots break down. If the result is normal and your clinical score is low, PE is almost certainly ruled out - with 97% accuracy. But here’s the catch: D-dimer goes up with age, pregnancy, infection, or cancer. So if you’re over 50, a normal D-dimer doesn’t mean much. It’s not reliable enough to rule out PE alone in older adults or those with cancer.
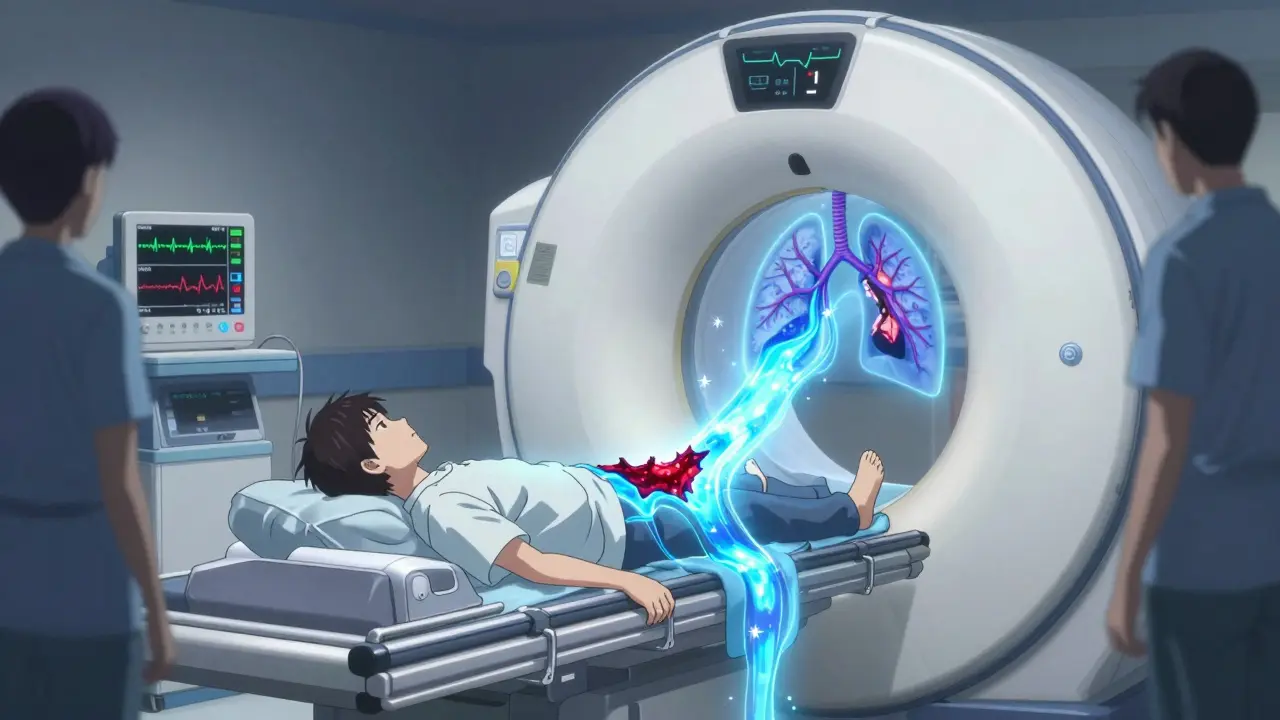
Step 3: CT Pulmonary Angiography (CTPA)
This is the gold standard. A CT scan with contrast dye shows exactly where the clot is. It finds PE in 95% of cases. The scan takes minutes. You lie on a table, get a quick IV injection, and the machine takes detailed images of your lung arteries. Radiation exposure is low - about the same as a cross-country flight. It’s safe, fast, and accurate.
Some people can’t have contrast dye due to kidney problems or allergies. In those cases, doctors use a V/Q scan - a nuclear medicine test that checks airflow and blood flow in the lungs. It’s not as sharp as a CT, but it still works well when contrast isn’t an option.
Step 4: Ultrasound for DVT
If you have leg swelling, doctors will often do an ultrasound of your legs. Finding a clot there confirms the source of the PE. It’s non-invasive, quick, and over 90% accurate. If you have a DVT, you almost certainly have a PE too - even if you didn’t feel lung symptoms.
What About Emergency Cases?
If someone is collapsing, has low blood pressure, or is in shock - this is a massive PE. Time is critical. In these cases, doctors don’t wait for scans. They use a bedside ultrasound of the heart (echocardiogram) to look for signs of right heart strain. If the right side of the heart is swollen and struggling, it means a large clot is blocking blood flow. That’s a code-red situation. Treatment starts immediately - often with clot-busting drugs or emergency procedures.
New Tools Making a Difference
Things are getting better. In 2023, AI tools like PE-Flow started helping radiologists interpret CT scans faster and more accurately - spotting tiny clots that humans might miss. These tools are now used in over half of major hospitals in the U.S. and Europe.
Another big change? Age-adjusted D-dimer thresholds. Instead of using the same cutoff for everyone, doctors now use higher thresholds for older patients. For example, someone who’s 75 has a normal D-dimer up to 850 ng/mL (instead of 500). This reduces unnecessary CT scans by more than a third - without missing real cases.
And then there’s the Pulmonary Embolism Response Team (PERT). These are specialized teams of doctors - radiologists, cardiologists, hematologists - who jump in within minutes when a serious PE is suspected. Hospitals with PERT programs have cut death rates by over 4%. That’s not just numbers - it’s lives saved.
What Happens After Diagnosis?
If PE is caught early, treatment is straightforward: blood thinners. Usually, you start with injections for a few days, then switch to pills. Most people take them for 3 to 6 months. Some - especially those with cancer or repeated clots - need them for life.
Recovery isn’t instant. You might still feel short of breath for weeks. That’s normal. Your lungs are healing. But if symptoms get worse - chest pain, dizziness, more swelling - you need to go back. Recurrence is real. One in three people who’ve had a PE will have another within 10 years.
What You Can Do
You can’t always prevent PE, but you can reduce your risk:
- Move regularly - even if you’re sitting for long flights or work. Stand up, walk, stretch your legs.
- Stay hydrated. Dehydration thickens blood.
- Know your history. If you’ve had a clot before, tell every doctor you see.
- Watch for leg swelling, pain, or warmth - especially after surgery or long trips.
- If you’re at high risk (cancer, recent surgery, genetic clotting disorder), ask about preventive blood thinners.
And if you ever have sudden, unexplained shortness of breath - don’t brush it off. Don’t assume it’s anxiety. Don’t wait to see if it gets better. Go to the ER. Get a D-dimer test. Get a scan. It could save your life.
Can pulmonary embolism happen without any symptoms?
Yes - but it’s rare. Small clots in the outer parts of the lungs might cause no symptoms at all. These are often found by accident during scans for other reasons. But when clots block larger arteries, symptoms are almost always present. Sudden shortness of breath is the most common warning sign. If you feel it, don’t ignore it.
Is pulmonary embolism the same as a heart attack?
No. A heart attack happens when blood flow to the heart muscle is blocked. A pulmonary embolism blocks blood flow to the lungs. They can feel similar - chest pain, shortness of breath, fast heartbeat - but they affect different organs. The treatments are completely different. Misdiagnosing PE as a heart attack can be deadly.
Can you have a pulmonary embolism and not know it?
You might not realize you had a small PE, especially if you had no major symptoms. But if you’ve had unexplained shortness of breath, leg swelling, or fainting, it’s likely you did. Many people only find out after a scan for another reason. The real danger is not knowing - because without treatment, another clot could form and be fatal.
How long does it take to recover from a pulmonary embolism?
Recovery varies. Most people feel better within weeks, but full healing can take months. Blood thinners reduce the risk of new clots, but your lungs need time to heal from the damage. Some people have lasting shortness of breath or lung pressure (called chronic thromboembolic pulmonary hypertension), especially if the clot was large or treatment was delayed.
Can you die from a pulmonary embolism?
Yes - and it happens faster than many people realize. About 1 in 10 people with undiagnosed PE die within the first hour. Most deaths happen before diagnosis. That’s why recognizing sudden shortness of breath and acting fast is so critical. With timely treatment, survival rates have improved dramatically - from 8.5% mortality in 2015 to 5.2% in 2022.

